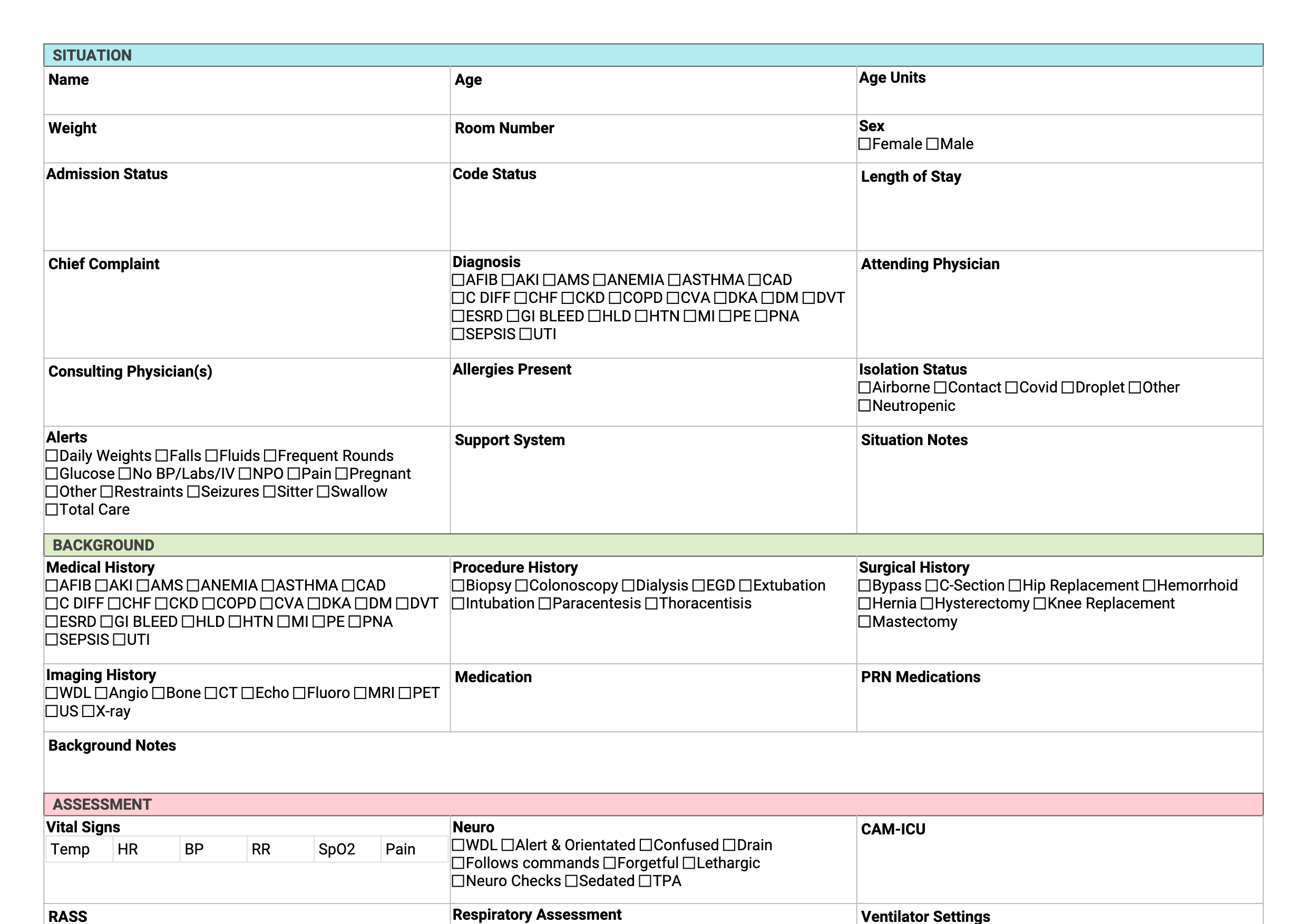
PICU nursing combines the complexity of pediatric care with the intensity of critical care — weight-based vasoactive drips, age-specific vent settings, neuro assessments calibrated for an infant versus a teenager, and families who are often experiencing the most terrifying days of their lives at the bedside. A good PICU brain sheet tracks all of it: the dose and rate of every drip, the vent parameters from the last RT rounding, which family member needs to be updated before rounds, and whether the 6-year-old's pain is controlled by FLACC or can now be self-reported. Download the free printable PDF below, or use the same template digitally in NurseBrain Synapse.
What is a PICU brain sheet?
The PICU merges every challenge of adult critical care with every variable of pediatric care. Your patient might be a 5 kg premature infant just transferred from the NICU with a cardiac defect, or a 40 kg teenager three days post-trauma. Every drip rate is weight-based. Every vent setting is age-adjusted. Every neuro check is developmental-stage-specific. And behind every patient is a family that needs clear, honest communication about a child who can't always speak for themselves. The PICU brain sheet is the tool that holds all of those variables in one place per patient so nothing gets missed in a 12-hour shift where the clinical picture can change hourly.
What to track on a PICU brain sheet
PICU brain sheets combine critical care and pediatric-specific tracking: weight in kg (current — every dose depends on it); age and developmental stage; diagnosis; neuro assessment (GCS or modified FLACC, pupils, sedation score); respiratory (vent mode and settings age-adjusted, SpO2, last ABG, ETT position); hemodynamics (HR, MAP, arterial line — with age-appropriate goals); weight-based vasoactive and sedation drips (name, rate, dose in mcg/kg/min, titration parameters); lines and access (site, date, size); I&O (hourly urine output with expected range for weight); labs; pending procedures; family communication notes; and pain management (scale used, score, last dose of analgesic).
PICU brain sheet vs PICU report sheet: same tool
Whether your unit calls it a brain sheet or a flow sheet, the PICU version needs to cover pediatric-specific fields that adult ICU sheets don't: weight-based dose calculation column, age-appropriate vital sign ranges, developmental pain scales, and family update tracking. The free PDF template covers these fields in one page per patient. NurseBrain Synapse is the digital version — track drip titrations, weight-based doses, vent adjustments, and family meetings digitally so your SBAR at shift change is accurate and complete.
PICU Nurse FAQ
What does a PICU nurse do?
A PICU nurse manages critically ill infants and children who need continuous monitoring and intervention. The clinical work looks like adult ICU — vasoactive drips, ventilator management, arterial lines, central access, frequent labs — but every parameter is weight-based and age-adjusted. You're also managing families in acute crisis: explaining complex diagnoses to parents who are often in shock, supporting siblings, and communicating prognosis in developmentally appropriate language for any children at the bedside. PICU nurses typically carry 1:1 or 1:2 assignments.
How does PICU differ from adult ICU nursing?
The core clinical difference is that PICU patients are not small adults. Every drip dose is calculated in mcg/kg/min and recalculated when weight changes. Vent settings, ETT sizes, normal vital signs, expected lab values, and fluid goals are all age- and weight-specific. Neuro assessments use developmental frameworks. Pain management uses age-appropriate scales. And the family is always present as part of the care team in a way that is more central in PICU than in most adult ICU settings.
What are normal vital signs for PICU patients?
Normal pediatric vital signs vary significantly by age. Neonates (0–28 days): HR 100–180, RR 30–60, systolic BP 60–90. Infants (1–12 months): HR 100–160, RR 30–60, systolic BP 70–100. Toddlers (1–2 years): HR 90–150, RR 24–40, systolic BP 80–110. Preschoolers (3–5 years): HR 80–140, RR 22–34, systolic BP 80–110. School age (6–12 years): HR 70–120, RR 18–30, systolic BP 85–120. Adolescents: approaching adult norms. Your PICU brain sheet should note the expected range for this child's age alongside each vital sign entry.
How do you calculate weight-based drips in the PICU?
PICU drip calculations use the formula: dose (mcg/kg/min) × weight (kg) × 60 min/hr = mcg/hr; then convert to mL/hr based on drug concentration. For example, a dopamine drip at 5 mcg/kg/min for a 10 kg child: 5 × 10 × 60 = 3000 mcg/hr. If the concentration is 1600 mcg/mL, the rate is 3000 ÷ 1600 = 1.875 mL/hr. Always verify with your hospital's pharmacy and weight-based drip calculator. Document the concentration, the dose in mcg/kg/min, and the resulting mL/hr on your PICU brain sheet.
Can I use a digital PICU brain sheet?
Yes. NurseBrain Synapse works on your phone or tablet. It's designed for bedside use and lets you track weight-based drips, age-adjusted vitals, developmental neuro assessments, and family communication notes for each PICU patient. Available on iOS and Android.